Drug and Alcohol Detox Center
Addiction and schizophrenia are two of the most misunderstood topics in mental health. Both carry heavy stigmas, are surrounded by myths, and can devastate lives if left untreated. When people ask whether addiction can cause schizophrenia, the answer isn’t simple. The truth is, addiction doesn’t directly cause schizophrenia, but substance abuse can trigger or worsen symptoms in someone who is already at risk. To understand this connection, it’s important to break down what schizophrenia is, how addiction affects the brain, and why the two conditions often appear side by side.
Schizophrenia is a serious mental health disorder that alters how a person thinks, feels, and perceives reality. Hallucinations, delusions, and disorganized thinking are common symptoms. It usually develops in late adolescence or early adulthood, and while the exact cause is unknown, researchers believe genetics, brain chemistry, and environmental stress all play a role. Schizophrenia isn’t caused by “bad behavior” or a lack of willpower—it’s a medical condition that requires treatment.
Addiction, on the other hand, hijacks the brain’s reward system. Substances like alcohol, cocaine, or meth flood the brain with dopamine, tricking it into craving more. Over time, this rewiring changes how the brain functions, making quitting extremely difficult without help. Addiction can cloud judgment, worsen mood, and push people to take risks they normally wouldn’t. When you combine addiction with an underlying vulnerability to schizophrenia, the results can be explosive.
One of the strongest links between addiction and schizophrenia is cannabis use. Studies show that heavy marijuana use, especially in teenagers and young adults, increases the risk of developing psychosis. While most people who smoke weed will never develop schizophrenia, those with a family history of the disorder face greater danger. For them, the drug can act as a trigger, flipping a genetic switch that brings schizophrenia symptoms to the surface. It’s not that marijuana “creates” the illness, but it can speed up its onset or intensify its severity.
Stimulants like cocaine and methamphetamine are also strongly tied to psychotic symptoms. People who abuse these drugs often experience paranoia, hallucinations, and delusions—symptoms that mimic schizophrenia. In some cases, these drug-induced psychotic breaks go away once the person detoxes, but in others, the symptoms linger, blurring the line between substance-induced psychosis and schizophrenia. It’s not uncommon for someone to be admitted to a hospital for what looks like drug-induced paranoia, only for doctors to later diagnose schizophrenia.
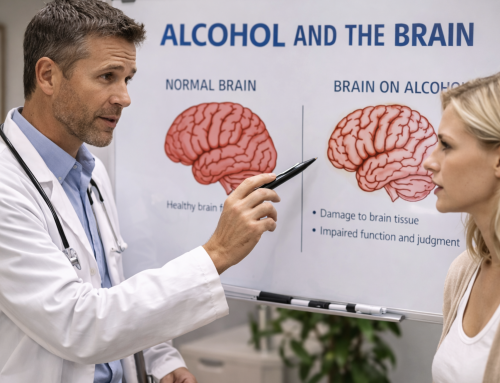
Alcohol, while legal and socially accepted, can also play a role. Long-term heavy drinking damages the brain and can cause severe psychiatric problems. Alcohol withdrawal, in particular, can bring on hallucinations and delusions, which can look like schizophrenia. For someone genetically vulnerable, the stress of alcohol misuse can be enough to worsen or expose underlying symptoms.
So, can addiction cause schizophrenia? The better way to put it is that addiction can unmask, accelerate, or worsen schizophrenia in people who are already predisposed. Addiction puts enormous stress on the brain, and when that stress is combined with genetic risk factors, it can lead to a breakdown in mental health. For some, the symptoms of schizophrenia may have appeared eventually no matter what. But substance abuse often speeds up the timeline and makes the illness more severe.
The relationship also works the other way around. Many people living with schizophrenia use drugs or alcohol to self-medicate. Hallucinations, paranoia, and racing thoughts are terrifying, and substances may offer a temporary escape. Unfortunately, self-medication usually makes symptoms worse in the long run. A person with schizophrenia who abuses substances often ends up with more frequent psychotic episodes, poorer treatment outcomes, and greater difficulty maintaining relationships or holding a job. This cycle can feel impossible to escape without the right help.
The overlap between addiction and schizophrenia highlights the importance of dual diagnosis treatment. Traditional rehab programs often focus only on substance abuse, while psychiatric care can focus only on mental health. But when both issues are present, treating one without addressing the other leaves a person vulnerable to relapse or worsening symptoms. Dual diagnosis programs bring together mental health professionals and addiction specialists to create a comprehensive recovery plan. Therapy, medication, peer support, and relapse prevention strategies all play vital roles in this type of care.
Another key factor is early intervention. The earlier schizophrenia is recognized and treated, the better the outcomes. The same is true for addiction. Unfortunately, stigma often keeps people from reaching out for help. Society tends to shame both conditions—labeling people with addiction as “weak” or those with schizophrenia as “crazy.” These harmful stereotypes prevent individuals from seeking the treatment they desperately need. Breaking down these barriers and encouraging open conversations about mental health and sobriety is essential.
Recovery is possible, even for those dealing with both schizophrenia and addiction. It isn’t easy—it requires patience, medical support, therapy, and often lifestyle changes—but people can and do rebuild their lives. Sobriety can bring clarity and stability, while treatment for schizophrenia can reduce symptoms and restore a sense of reality. Together, these steps offer hope and a path forward.
At the end of the day, addiction doesn’t directly cause schizophrenia, but it can create the conditions for it to emerge or become worse. Both conditions are serious and deserve compassion, understanding, and professional care. Instead of asking whether addiction causes schizophrenia, the better question is: how can we support people struggling with either, or both? The answer lies in treatment, community, and the belief that recovery—whether from substance abuse, mental illness, or both—is always possible.
Call us at 844-658-0927 or contact us today to speak with a member of our admissions team.